
Homepage - - - Tutorial Index
Genetic Diseases
Many are the hereditary diseases that affect the kidney, nevertheless, we will include here only those that, for reasons of somewhat arbitrary organization, we did not consider in other chapters: Alport Syndrome, thin basement condition, nail-patella syndrome, type III Collagen Glomerulopathy, lecithin-cholesterol acyltransferase deficiency, Fabry disease, Gaucher disease, other lysosomal diseases, glycogen storage disease type I, Fanconi syndrome (and Lowe syndrome), Barter syndrome y fibronection glomerulopathy.
It is a hereditary syndrome in which there are abnormalities of type IV collagen and which is characterized by progressive renal failure, sensorineural deafness and ocular alterations. About 85% of cases are transmitted as X-linked inheritance (Xq22) due to the mutation in the COL4A5 gene that encodes the alpha-5 chain of type 4 collagen. The type IV collagen in the glomerular basement membrane (GBM) is formed, in addition, by the alpha-3 and alpha-4 chains and we can find mutations in the genes that encode them (COL4A3 and COL4A5, in 2q35-37) in cases of Alport transmitted in an autosomal manner (recessive in 14% of cases) and dominant at 1%).
The genes COL4A1 to COL4A6 encode six chains that only form three sets of triple helices that are designated: alpha-1.alpha-1.alpha-2 (IV) that appears in fetal glomerular capillaries but is gradually replaced by alpha-3.alfa -4.alpha-5 (IV) in mature glomerular capillaries; and alpha-5.alpha-5.alpha-6 (IV) that appears in Bowman's capsule, skin, smooth muscle, and esophagus. Alpha-3.alpha-4.alpha-5 (IV) is also found in basal distal renal tubules, lungs, testicles, cochlea and eye.
The replacement of alpha-1.alpha-1.alpha-2 (IV) by Alpha-3.alpha-4.alpha-5 (IV) is a critical process in the maturation of the kidney. Mutations in COL4A3, COL4A4 or COL4A5 produce a defect in the assembly that prevents the formation of type IV collagen and, therefore, there is no normal replacement of fetal IV collagen. This collagen is less resistant against proteases, physical stress and oxidants to which the GBM is exposed and, contrary to the collagen IV of the normal glomerulus, it undergoes proteolysis and this degradation produces irregular thickening, cracking and multilamination. This damage allows the filtration of erythrocytes and plasma proteins through the GBM. Presumably a slight defect would produce only thinning of the GBM (Kashtan C. Alport syndrome: facts and opinions. F1000Res. 2017;17;6:50. [PubMed link]; Cosgrove D, Liu S. Collagen IV diseases: A focus on the glomerular basement membrane in Alport syndrome. Matrix Biol. 2017;57-58:45-54. [PubMed link]; Torra R, et al, Collagen type IV (alpha3-alpha4) nephropathy: from isolated haematuria to renal failure. Nephrol Dial Transplant. 2004 Oct;19(10):2429-32. [PubMed link]; Hudson BG, et al Alport's syndrome, Goodpasture's syndrome, and type IV collagen. N Engl J Med. 2003 Jun 19;348(25):2543-56. [PubMed link] [Free full text]). The incidence of Alport syndrome is approximately 1 in 5,000 people.
Clinical features: Men are more frequent and more severely affected than women who are heterozygous and have mosaicism of the altered gene product (in each cell, an X chromosome is inactivated randomly). Virtually all men develop terminal renal failure at some point in their life; in women it does not usually occur, although it rarely occurs; in most of them there are slight abnormalities, only in 10-15% there is no clinical evidence of the disease. There may be no family history due to new mutations, lack of clinical manifestations in the carriers and autosomal recessive variants.
In men there is persistent microscopic hematuria from the first years of life, this may be accompanied by episodes of macro hematuria after respiratory infections. In women, there is usually intermittent microscopic hematuria. Proteinuria usually appears later and becomes progressively larger; there is proteinuria in the nephrotic range in 30-40% of adult patients. The fall in creatinine clearance begins to be evident towards the second decade of life in men and is associated with proteinuria and hypertension. Some authors have classified it into a juvenile variant: renal failure before age 31, and adult variant: renal failure after age 31.
Sensorineural deafness begins to develop towards the middle of the second decade of life; initially it is only detected by audiometry. In women there is usually no deafness and in some families it does not occur. There are eye defects in 15-30% and include: anterior lenticone (conical protrusion of the central portion of the lens in the anterior chamber), pigmentary changes of the retina and alterations of the cornea.
There is no treatment for the disease except kidney transplantation. End-stage renal failure usually occurs between the third and fifth decades of life. Many of the patients lack the antigen against which the antibody of the anti-MBG disease is directed and after the transplant the immune system detects it producing glomerular damage. These anti-bodies are detected in 30% of transplanted patients, but glomerulonephritis occurs only in 3-4%; it is less frequent in patients who did not have deafness. See Case 134 of our Case series: anti-GBM disease in a kidney transplanted patient due to Alport syndrome.
Laboratory findings: The main findings are hematuria and proteinuria. There is progressive increase in creatinine with increasing age. Studies for immunological alterations are negative. No other specific findings.
Histopathology
The microscopic changes are nonspecific and may simply reflect the chronic glomerular and tubulo-interstitial damage. Electron microscopy is necessary for diagnosis.
There is a slight increase in the matrix and mesangial cellularity that can be progressively increased. In silver-methenamine stains, thickening of the capillary walls and, in some cases, multilamination can be evidenced. The Bowman capsule appears with varying degrees of thickening. In more advanced stages there is global sclerosis of glomeruli and we can also see segmental sclerosis, sometimes with hyalinosis. In young men we can see small glomeruli with few capillaries giving an appearance called "fetal".

Figure 1. The alterations of the glomerular basement membrane in the Alport syndrome can not be evidenced clearly in the conventional histological study; In some cases we can see irregularities of the capillary wall (arrows), with areas of thick appearance, thinner areas and, in some cases, laminated aspect of it. (Methenamine-silver, X1,000))
In tubules we can find erythrocytes, protein reabsorption droplets and other nonspecific changes such as atrophy. In the interstitium clusters of foamy histiocytes have been classically described, often near the corticomedullary junction, which are not specific to the disease and can be seen in any patient with proteinuria in the nephrotic range. (See image [link]). In advanced stages there is fibrosis and chronic inflammation. In vessels there are no specific changes.
Immunofluorescence
It is usually negative. Segmental deposits of IgM and C3 can be found by nonspecific entrapment, as in other causes of focal and segmental glomerulosclerosis, these do not represent an immunological mechanism of injury.
Immunohistochemistry
To determine the type of inheritance, immunohistochemistry can be used to detect chains of type IV collagen. If there is absence of staining for alpha-5 (IV) in the epidermal basement membrane or absence of staining for alpha-3 (IV), alpha-4 (IV) and alpha-5 (IV) in distal renal tubules and glomerular capillaries, this is the characteristic finding in X-linked Alport. If there is absence of staining for all three chains in the GBM and distal tubules with staining for alpha-5 (IV) in Bowman's capsule suggests Alport with autosomal inheritance.

Figure 2. IF to detect alpha-3 chain of type IV collagen. Note the linear staining in glomerular basement and distal tubule membranes: Normal. In Alport disease is almost always negative (both in cases with X-linked inheritance and autosomal inheritance). original magnification, X200.

Figure 3. IF to detect alpha-5 chain of type IV collagen. Linear staining in glomerular basement membranes, distal tubules and Bowman's capsule: Normal. In X-linked Alport disease there is negativity. In autosomal Alport staining in MBG and tubules is lost and it is preserved in the Bowman capsule. Original magnification, X200.

Figure 4. Normal staining for alpha-5 chain of type IV collagen in skin. In X-linked Alport is negative. In the skin there is no expression of alpha-3 or alpha-4 chains, so it is not useful for the diagnosis of autosomal Alport. IF for alpha-5 (IV), original magnification, X400.
Electron microscopy
The characteristic change in men consists of diffuse irregularities of the GBM with variation in the thickness and variable appearance of the dense lamina, with lucid and electron-dense zones that give it a basket and multilaminated appearance; there may be finely laminar material in the lucid zones. There are zones of frank thickening that alternate with other thinned ones; defects are detected due to discontinuity of the GBM, which causes the endothelial and epithelial cells to appear almost together. In young men and in women there may be a diffuse thinning without the multilaminated appearance of adults, with changes similar to those of thin basement membrane condition. There may be similar changes in the basal tubular membranes and Bowman's capsule. As glomerular disease progresses there is usually progressive loss (or fusion) of podocyte processes.

Figure 5. Irregular basement membranes, with laminations, very thickened areas alternating with very thin ones. EM, original magnification, X4,000.

Figure 6. In this image, the laminations of the basement membrane are more evident in a case of X-linked Alport. Original magnification, X4,000.
[See a revision in eMedicine© (link)]
See Case 94 of our Case Series. - See Case 100 of our Case Series. - See Case 124 of our Case Series.
GLOMERULAR THIN BASEMENT MEMBRANE CONDITION (TBMC).
Also called "thin basement membrane disease", "thin basement membrane nephropathy", "thin basement membrane lesion", "thin basement membrane syndrome". Many of the patients with this disorder have hematuria, have a family history of the same disease and a benign course, which is why it has also been known as "benign familial hematuria", however, this name is no longer favored and lends confusion to other diseases that occur with hematuria; In addition, the course is not always benign. Other terms that have received the disease have been: "benign essential hematuria" and "persistent benign hematuria". It is characterized by microhematuria (usually persistent), mild proteinuria, normal renal function, diffuse thinning of the GBM and, in many cases, a family history of hematuria.
It had been suspected that the genetic defect in thin basement membrane condition (TBMC) would be similar to that in Alport syndrome since patients with the latter group of disorders also have thin glomerular basement membranes (GBM) early in the course of the disease. This hypothesis was confirmed in families in which TBMN was associated with heterozygous defects in COL4A3 or COL4A4, the genes that encode the alpha-3 and alpha-4 chains of type IV collagen (Savige J et al, Thin basement membrane nephropathy. Kidney Int 64:1169-78, 2003. [PubMed link]). Patients with TBMC can be considered "carriers" of autosomal recessive Alport syndrome since mutations in both alleles of COL4A3 or COL4A4 cause autosomal recessive Alport syndrome. Mutations in both alleles can be the same (homozygous) or different (compound heterozygous). Approximately 40 to 50 percent of heterozygous carriers of a COL4A3 or COL4A4 mutation in Alport families exhibit microhematuria. Although both alleles of COL4A3 or COL4A4 must be involved to produce autosomal recessive Alport syndrome, TBMC is transmitted in a dominant fashion because the abnormal gene product produces a defect in collagen that is sufficiently severe to interfere with the normal architecture of the GBM, resulting in hematuria. In most cases, however, the heterozygous defect does not provoke the secondary processes that result in the proteinuria, impaired glomerular filtration, and renal fibrosis observed in patients with Alport syndrome. Linkage with the COL4A3 and COL4A4 genes has not been found in all families with TBMC, the underlying defect(s) in these other families are not known, possibilities include de novo mutations, incomplete penetrance, or novel genetic loci (Kashtan C. Thin basement membrane nephropathy (benign familial hematuria). In UpToDate [Link]. Consulted on 29 November 2017). Some cases diagnosed as TBMC may be associated with other glomerulopathies, as focal segmental glomerulosclerosis, IgA nephropathy, membranous GN etc. (Savige J et al, Thin basement membrane nephropathy. Kidney Int 64:1169-78, 2003. [PubMed link]).
TBMC is probably the most frequent cause of persistent or recurrent isolated hematuria in children and adults and its prevalence varies according to different series (and perhaps in different populations) (Savige J, et al, Thin basement membrane nephropathy. Kidney Int 64:1169-78, 2003. [PubMed link]).
Some families with clinical presentation of benign familial hematuria may have a "normal" thickness of the GBM.
Clinical features: The main feature is microscopic hematuria that begins in childhood, is usually persistent but may be intermittent; in some cases there is gross hematuria but it is not usual, and, according to Kern et al, could be cases of another glomerulopathy (such as IgA nephropathy) not fully studied (Kern WF, et al, Atlas of Renal Pathology. W.B. Saunders Company, Philadelphia, 1999, p. 235-246). There is usually no proteinuria or it is minimal; proteinuria greater than 500 mg/24 hours suggests another diagnosis or worse prognosis (Savige J, et al. Kidney Int 64:1169-78, 2003. [PubMed link]). Renal function is normal in the great majority of cases; however, TBMC is not always a benign disease, in some cases there is important proteinuria, occasionally nephrotic syndrome, and alterations in renal function. Such patients may have unrecognized Alport syndrome, represent a more severe phenotype of TBMC, or have another gene polymorphism influencing their course (Kashtan C. Thin basement membrane nephropathy (benign familial hematuria). In UpToDate [Link]. Consulted on 29 November 2017).
Histopathology
There are no histological alterations in conventional light microscopy. We can see erythrocytes in Bowman's space and/or in tubules. In some cases there are focal and segmental glomerulosclerosis lesions, which is an adverse prognostic factor (unrecognized Alport?). In other cases IgA nephropathy is documented, but the relationship between the two diseases is not very clear, it could be a collision of diseases rather than a pathogenic relationship.
Immunofluorescence
It is characteristically negative. We can find traces of some immunoglobulins or complement fractions, but nothing specific (except if there is another concurrent glomerulopathy).
Electron Microscopy
There is diffuse and global thinning of the MBG, its contours are smooth and there is no multilamination. In some cases we see some irregularity or stretches of GBM with normal thickness. The biggest problem is that there is no exact value, universally accepted, for the thickness of the MBG. This thickness varies with age, being progressively greater until adulthood; It is higher in men and there are changes according to the tissue processing. Each laboratory must determine its range of "normal" values by age and sex (Dische FE, Measurement of glomerular basement membrane thickness and its application to the diagnosis of thin-membrane nephropathy. Arch Pathol Lab Med 116:43-9, 1992. [PubMed link]). The measurement should be made from the outer surface of the endothelial cell to the inner surface of the visceral epithelial cell, in a microphotograph with a known magnification. Some authors use a limit of 300 nm and others of 250 nm to diagnose MBD in adults. The diagnosis should be made with great caution in children, given the lower thickness of the GBM in these patients.

Figure 7. Diffuse thinning of the glomerular basement membrane in a case of TBMC. There are no irregularities or laminations and the thinning is relatively homogeneous. The average thickness was 180 nm. ME, original magnification, X6.000.

Figure 8. Another case of TBMC with diffuse thinning of the GBM, in a teenager with persistent microghematuria, ME, original increase, X5,000.

Figure 9. Measurement of the basement membrane in the biopsy of a patient with TBMC. ME, original magnification, X8.000.
If we take the mean +/- 1.5 times the standard deviation (SD) of the thickness of the MBG in a normal population, the lower values of this range can be superimposed with those of the thickness of patients with TBMC and these low values are Found mainly in women (Dische FE, Measurement of glomerular basement membrane thickness and its application to the diagnosis of thin-membrane nephropathy. Arch Pathol Lab Med 116:43-9, 1992. [PubMed link]) which indicates that we should be cautious with the diagnosis (Lajoie G, Approach to the diagnosis of thin basement membrane nephropathy in females with the use of antibodies to type IV collagen. Arch Pathol Lab Med 125:631-6, 2001 [PubMed link / Free full text link]).
See Case 140 of Our Case Series: TBMC.
Also called hereditary osteo-onychodysplasia. It is a hereditary disease characterized by dysplasia of the nail bed, hypoplasia or absence of the patella, deformity or subluxation of the head of the radius, abnormalities of the pelvis and alterations of the MBG.
Mutations in the LMX1B gene cause nail-patella syndrome. The LMX1B gene provides instructions for producing a protein that attaches (binds) to specific regions of DNA and regulates the activity of other genes. On the basis of this role, the LMX1B protein is called a transcription factor. The LMX1B protein appears to be particularly important during early embryonic development of the limbs, kidneys, and eyes. Mutations in the LMX1B gene lead to the production of an abnormally short, nonfunctional protein or affect the protein's ability to bind to DNA. It is unclear how mutations in the LMX1B gene lead to the signs and symptoms of nail-patella syndrome (Nail-Patella Syndrome. In Genetics Home Reference. Consulted on 29 November 2017 [LINK]).
It is an uncommon disease, it occurs in approximately 22 people per million.
Clinical features: The most frequent findings are proteinuria, sometimes in the nephrotic range, microscopic hematuria, edema and hypertension. There are nail abnormalities in 80-90%, most often in the fingernails. There are abnormalities of the iliac crests: anterior and posterior iliac spines prominent in 80% (this abnormality can be pathognomonic in some cases) and abnormalities of the patella in 60%. Alterations in the elbow are less frequent. With some frequency there are malformations of the urinary tract.
In more than half of patients there are no renal alterations; In those who do, the disease is usually mild, but about 10% will reach terminal renal failure.
Histopathology
There are no alterations or these are nonspecific. There may be global or segmental glomerulosclerosis, nonspecific vascular and tubulointerstitial changes. In some cases the GBM may have a slight thickening.
Immunofluorescence
It is negative, or there is entrapment of IgM, C3 or C1q in segments with sclerosis.
Electron Microscopy
The GBM has electrolucid areas that give it a moth-eaten aspact, these areas are more prominent in areas of thickened GBM. Electron-lucid areas can also be seen in the mesangium, where we will find a slight increase in the mesangial matrix. The lucid zones contain small, dark, coarse, collagen-like fibers; they are difficult to visualize and, sometimes, require tissue staining with phosphotungstic acid. The collagen fibers are seen towards the central part of the GBM. In tubular basal membranes these changes are not observed. In podocytes we can see simplification of their cytoplasmic processes. [See EM image - Link]
TYPE III COLLAGEN GLOMERULOPATHYIII
Also called collagenofibrotic glomerulopathy. It is characterized by accumulation of fibrillar collagen in the extracellular glomerular matrix, initially, it was considered to be related to the nail-patella syndrome, but it is currently considered a different disease. It is more frequently reported in Japan.
Although the etiology and physiopathogenic mechanism of the disease are not well known, it seems to be an autosomal recessive genetic defect, but there are sporadic cases, in some cases it is associated with factor H deficiency. In these patients there is an increase in the serum concentration of the procollagen peptide III, its determination in serum is a very good diagnostic aid.
In the human kidney, type III collagen, a structural protein of the extracellular matrix, is present only in the interstitium and blood vessels and not in the glomerulus. Accumulation of type III collagen fibrils within the mesangial matrix and subendothelial space is a typical feature of collagen type III glomerulopathy (Dong J, Wei H, Han M, Guan Y, Wu Y, Li H. Collagen type III glomerulopathy: A case report and review of 20 cases. Exp Ther Med. 2015;10(4):1445-1449. [PubMed link]).
Clinical features: It affects both sexes equally; it presents with persistent proteinuria, with or without haematuria; In some families, isolated microscopic hematuria is described. It usually begins in childhood, in many cases proteinuria is progressive and end-stage renal damage can develop. In adults there may be a more indolent course. There are no the extrarenal manifestations of the nail-patella syndrome.
Histopathology
There is a marked increase in the glomerular tuft due to expansion of the mesangial matrix and thickening of capillary walls. With the PAS it is noted that the thickening is due to the presence of poorly stained subendothelial material and mesangial interposition. The lesion may resemble capillary wall lesions in thrombotic microangiopathy or, if there is mesangial hypercellularity, to type I membranoproliferative GN . (Several images in: Duggal R, et al. Collagenofibrotic glomerulopathy-a review. Clin Kidney J. 2012;5(1):7-12. [Full text link]).
Immunofluorescence
Negative or unspecific deposits of IgM and C3.
Immunohistochemistry
There is strong mesangial and capillary walls staining for collagen type III, which is normally absent from the extracellular matrix. In cases of glomerular sclerosis, there is focal distribution of this collagen, contrary to type III collagen glomerulopathy in which it is diffuse and global.
Electron Microscopy
The mesangial matrix and the subendothelial space of the GBM are enlarged and with a mottled appearance. There are bands of fibrillar collagen that become more noticeable with phosphotungstic acid. These accumulations can be large, located in mesangium and subendothelial space and, characteristically, in the vast majority of cases, the dense lamina is preserved.
(Several images in: Duggal R, et al. Collagenofibrotic glomerulopathy-a review. Clin Kidney J. 2012;5(1):7-12. [Full text link] [PubMed link]).
LECITHIN-CHOLESTEROL ACYLTRANSFERASE (LCAT) DEFICIENCY
It is a rare inherited autosomal recessive disease in which there is a deficiency in the esterification of plasma cholesterol, the increased plasma concentration of unesterified cholesterol, triglycerides and phosphatidylcholine results in tissue deposits of lipids. The disease was initially described in Norway, but it has a wide distribution in the world.
The two familial forms of LCAT deficiency are termed familial LCAT deficiency (complete LCAT deficiency) and fish eye disease (partial LCAT deficiency). Familial LCAT deficiency, first reported in 1967 in a Norwegian family, is characterized by the absence of LCAT activity towards HDL and LDL. Fish eye disease, initially described in two families of Swedish origin, is characterized by the absence of LCAT activity towards HDL only. Familial LCAT deficiency and fish eye disease are both autosomal recessive disorders caused by mutations of the LCAT gene. Only one LCAT gene has been discovered, with certain mutations of the gene resulting in familial LCAT deficiency and other mutations of the gene causing fish eye disease. The exact location of the mutations of the LCAT gene cannot yet be used to predict the clinical or biochemical manifestations of either familial LCAT deficiency or fish eye disease (Anastasopoulou C.Lecithin- Cholesterol Acyltransferase Deficiency. In: eMedicine, consulted on 30 November 2017 [Link]).
Clinically there are opacities in the cornea, hemolytic anemia, accelerated arteriosclerosis and proteinuria with renal failure. Kidney involvement begins with proteinuria in childhood and ends, after several decades, in renal failure, it is the main cause of morbidity and mortality. Usually there is hematuria, leukocyturia and cylindruria. Kidney failure does not occur in all cases. The corneal opacities may suggest the disease (One image in: Marin G, et al. Acta Med Colomb 2006; 31(4): 422-426 [Full text link]).
Histopathology
The glomeruli are the main site of injury. There is mesangial expansion and thickening of capillary walls. There are foamy cells in mesangium and capillaries and small holes are seen in the capillary walls, giving an aspect of membranous GN (Figures 10 and 11). You can also see images in double contour and "spikes". There may be segmental sclerosis. In the interstitium we can also find foam cells.

Figure 10. Foam cells, areas with empty appearance and intracapillary hyaline accumulations, which give an unusual appearance to the glomerulus, alterations very suggestive of LCAT deficiency. (H&E, X400).

Figure 11. Irregular capillary walls, with holes. Sometimes we can see spikes that suggest membranous GN; double contours can also be seen, with appearance of membranoproliferative GN. (Methenamine-silver, X400)
Immunofluorescence
Negative or unspecific immunostaining in sclerosing lesions.
Electron Microscopy
Lipid deposits are identified in mesangium and capillary walls: subendothelial, subepithelial and intramembranous. The lipids are partially lucid and partially osmophilic, with fibrillar appearance, with striations, curvilinear and sinuous. These deposits can also be found in the endothelium of arterioles and arteries, and in its middle layer. (Several images in: Marin G, et al. Nephrotic syndrome secondary to lecithin-cholesterol acyltransferase deficiency Case report. Acta Med Colomb 2006; 31(4): 422-426 [Full text link])
Deposits recur post-transplant but are not necessarily associated with graft dysfunction.
See Case 95 y See Case 110 of our Case Series.
Also called "angiokeratoma corporis diffusum universale" and Anderson-Fabry disease. It is a X-linked hereditary metabolic disease caused by deficient activity of the lysosomal enzyme alpha-galctosidase A (alpha-Gal A). This deficiency results in progressive lysosomal accumulation of glycosphingolipids (GSL), derived from the turnover of cells, mainly in kidneys, liver, lungs and erythrocytes. The genetic defect is located in Xq22 and occurs in all types of cells, but the involvement is different in each organ. Clinical manifestations depend, in large part, on the accumulation of GSL in the endothelium and, to a lesser degree, in other types of cells.
There are multiple mutations described for this disorder, some more associated with renal variants and others with cardiac variants of the disease, however, there is a wide phenotypic variety and the clinical manifestations can not be predicted by the type of mutation.
Clinical features: Main manifestations in homozygous are: angiokeratomas (skin), hypohidrosis, severe pain crisis in extremities (acroparesthesia), cornea and lens opacities, cardiac involvement, cerebrovascular manifestations and renal dysfunction.
Women who are heterozygous may remain asymptomatic during all or a large part of their lives, but in some cases there are obvious signs of the disease and there may even be severe disease.
Cardiac and renal variants have been described. In the first, the effectation is predominantly of the heart, with little or no renal and systemic involvement, sometimes only with left ventricular hypertrophy. In the renal variant, the kidneys are the most affected organs and it is believed that a significant percentage of patients with terminal renal failure of unknown cause (up to 1% of the total) can have this variant of the disease; in many cases it is never diagnosed.
The clinical keys for diagnosis are mainly extrarenal: skin and eye lesions, therefore, in renal and cardiac variants the diagnosis can be never recognized. Some authors suggest measuring the activity of the enzyme in all patients with chronic renal failure of unknown etiology.
The diagnosis is confirmed by measuring the activity of alpha-Gal A in plasma or leukocytes. In homozygous, activity is usually not detected or it is less than 1%, in heterozygotes there may be a variable percentage of activity, but it is almost always diminished .
Histopathology
The most striking changes are in glomeruli; The podocytes are large and vacuolated, with hypertrophic appearance and cytoplasm distended by vacuoles that give them a foamy appearance. They are empty in conventional cuts from paraffin- embedded tissue because the GSL are lost with routine processing. If the tissue is pretreated with osmium the GSL are conserved. In freeze-cut material (still fixed in formaldehyde), intracytoplasmic inclusions appear birefringent, autofluorescent and sudanophilic, they are also positive with the PAS. We can also find this material in mesangial, tubular and interstitial cells. In the endothelium of arteries and arterioles there are cytoplasmic inclusions and, as an important feature, there is usually no renal endothelial cell involvement in the cardiac variant of the disease, this would help to differentiate it from the renal variant, where they are abundant. Other renal changes are nonspecific and are related to chronic damage.
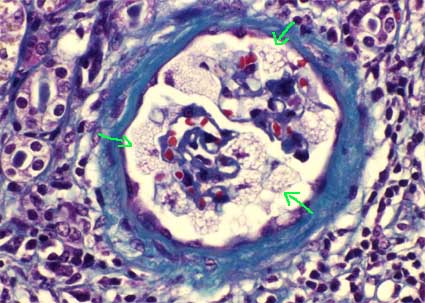
Figure 12. In Fabry's disease, the vacuolated aspect of podocytes is very characteristic, which gives a very particular appearance to the glomeruli (arrows). We can also see vacuolated cells in the tubular epithelium, Bowman's capsule and in endothelium. (Masson's trichrome, X400).

Figure 13. In sections of tissue fixed in formalin and treated with osmium, to preserve glycosphingolipid deposits, it is possible to see the material accumulated in the cytoplasm of podocytes and other cells. Note the extensive inclusions of glycolipids in podocytes with some deposits in tubular cells (arrow). (Kidney biopsy fixed in formaldehyde, then treated with osmium and stained with fast green, X400).
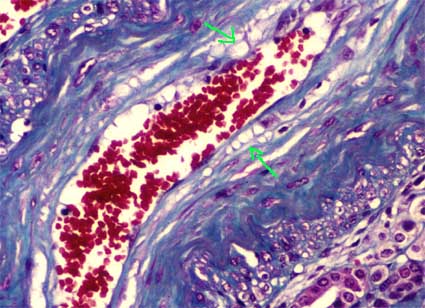
Figure 14. Deposits of glycosphingolipids in endothelial cells of an artery evidenced as extensive vacuolization of their cytoplasm (arrows). (Masson's trichrome, X400).
Immunofluorescence: Negative or unspecific.
Electron Microscopy
There is osmophilic material, laminated, similar to myelin bodies; they are mainly found in podocytes, epithelium of Bowman's capsule, tubular epithelium and endothelium, although they can be seen in any type of cells. Myelin-like bodies have a periodicity of 4 to 10 nm.

Figure 15. Electron microscopy of the same case of the three previous microphotographs showing a podocyte with laminated structures in its cytoplasm: "myelin bodies". (Electron microscopy, original magnification, X4,000).
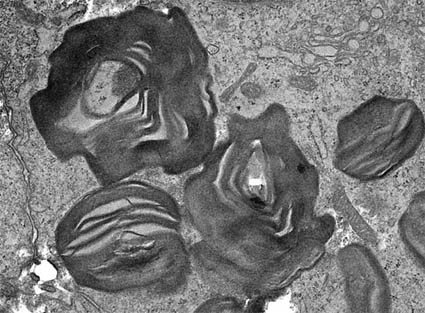
Figure 16. Another image of GSL inclusions in podocytes. (Electron microscopy, original magnification, X8,000) .

Figure 17. Inclusion in podocyte of a woman with Fabry disease and severe clinical alterations. (Electron microscopy, original magnification, X8,000).
In kidney grafts, although there is normal enzyme in their cells, GSL can be deposited in endothelial cells, but usually does not cause kidney damage. Even so, treatment with enzyme replacement must be done to avoid alterations in other organs.
In 2005, we published an interesting case of a renal variant of the disease associated with conventional bilateral renal carcinoma. (Blanco J, Herrero J, Arias LF, et al, Renal variant of Anderson-Fabry disease and bilateral renal cell carcinoma. Pathol Res Pract 200:857-60, 2005. [PubMed link])
See Case 125 of our Case Series.
It is another genetic disease due to storage of sphingolipids, it is caused by deficiency of the acid lysosomal beta-glucosidase enzyme and produces accumulation of glucosyl ceramide. This material accumulates in many organs and produces hhepatosplenomegaly, pancytopenia and degenerative bone changes, without neuropathy in the type I. In the kidney they produce proteinuria and, sometimes, renal failure, but it is not usual. Reports of renal abnormalities in patients with Gaucher disease are limited to case reports.
Microscopically, it is characterized by the accumulation of foam cells in many organs such as the bone marrow, liver and spleen. In the kidney there are accumulations of these lipids in the glomerular endothelial cells and mesangial cells. This lipid is not lost with paraffin processing; it is weakly positive with PAS and moderately positive with black Sudan (lipid staining).
By electron microscopy, the inclusions have microtubular appearance and are surrounded by membrane. The endocapillary cells of Gaucher are probably monocytes and have pseudopodia that extend into the subendothelial space. Occasionally there are cells with inclusions in the interstitium.
OTHER LYSOSOMAL STORAGE DISEASES include nephrosialidosis (produces proteinuria and early kidney damage) due to deficiency of lysosomal alpha-neuraminidase glycoprotein-specific; gangliosialidosis; I-cell disease (mucolipidosis type II) and Hurler's syndrome.
GLYCOGEN STORAGE DISEASE TYPE I
Or von Gierke's disease, is produced by deficiency of glucose-6-phosphatase (G-6-Pasa). There is an increase in kidney size since childhood with subsequent development of proteinuria and hypertension. There is glomerular hyperfiltration and there may be an incomplete form of renal tubular acidosis.
The glomeruli are hypertrophic and contain large amounts of mesangial lipids. The tubules have large cells, vacuolated and filled with glycogen. Progressively, glomerular sclerosis and tubulointerstitial damage develop.
It is characterized by aminoaciduria, glucosuria and phosphaturia, affected children develop hypophosphatemia and rickets resistant to vitamin D (glucoaminophosphodiabetes). In adults there is osteomalacia. It is a heterogeneous disorder of tubular transport. It commonly includes proximal tubular acidosis, alterations in urine concentration and altered potassium, urate and citrate reabsorption. It can present as a primary disease (also called Toni-Debré-Fanconi syndrome) or as a secondary manifestation of other hereditary and acquired diseases.
In the primary Fanconi syndrome there may be autosomal dominant, autosomal recessive and X-linked inheritance. Sporadic cases are also described. Another related syndrome is the so-called Dent disease, Dent disease is an X-linked recessive disorder of the proximal tubules that is characterized by low-molecular-weight proteinuria, hypercalciuria, nephrocalcinosis, kidney stones, renal failure, and rickets [1,2]. In most cases, it is due to mutations that inactivate a voltage-gated chloride transporter named CLC-5. In others, it is associated with mutations in the OCRL1 gene, which is also mutated in the oculocerebrorenal syndrome of Lowe. Further genetic heterogeneity is assumed to exist since there are patients with the distinctive phenotype of Dent disease without mutations in either of these genes (Scheinman SJ. Dent disease (X-linked recessive nephrolithiasis). In: UpTo Date, consulted on Dec 4, 2017 [Link]).
The secondary Fanconi syndrome is more frequent than the primary one. It can occur in cystinosis (the most common cause), tyrosinemia, galactosemia, hereditary fructose intolerance, hepatorenal glycogenosis, Wilson's disease, and Lowe's oculocerebral syndrome.
Histopathology
In Fanconi syndrome, of any cause, the most prominent alteration is tubular atrophy with interstitial fibrosis, variable inflammation and progressive glomerular sclerosis. Tubular atrophy is more pronounced in the first part of the proximal tubule in which a "swan neck" appearance has been described, due to the shortening and narrowing of the postglomerular segment (it is not specific to Fanconi). The most initial changes are the loss of the brush border and the shortening of the cells, although this seems to be a secondary change, rather than the cause of the tubular alterations. We can see cellular vacuolization and calcification of the tubular basal, probably as a consequence of hyperparathyroidism due to renal failure. The Armanni-Ebstein lesion (large accumulations of glycogen in the right pars of proximal tubules) is another finding, although not very common, and of unknown cause (it can also be found in diabetic nephropathy).
If there is cystinosis we will see the characteristic interstitial crystals (they dissolve with paraffin processing and freeze cuts are needed). In Dent's disease we see many tubular and interstitial deposits of calcium monophosphate (basophilic).
LOWE SYNDROME or oculocerebrorenal syndrome is a hereditary X-linked disease characterized by congenital ocular abnormalities (microphthalmos, cataracts, glaucoma), severe brain dysfunction and renal tubular dysfunction: Fanconi syndrome.
There are other tubular genetic defects that do not usually give morphological alterations and that are related to alterations in the transport of glucose, aminoacids or ions.
Bartter syndrome represents a set of closely related, autosomal recessive renal tubular disorders characterized by hypokalemia, hypochloremia, metabolic alkalosis, and hyperreninemia with normal blood pressure. The underlying renal abnormality results in excessive urinary losses of sodium, chloride, and potassium. Bartter syndrome has traditionally been classified into three main clinical variants: Neonatal (or antenatal), Classic and Gitelman syndrome. Others have divided Barter syndrome into 5 types. Advances in molecular diagnostics have revealed that Bartter syndrome results from mutations in numerous genes that affect the function of ion channels and transporters that normally mediate transepithelial salt reabsorption in the distal nephron segments. Hundreds of mutations have been identified to date. Symptoms include the following: Polyuria, polydipsia, vomiting, constipation, tendency for volume depletion, failure to thrive, linear growth retardation. Other symptoms, which appear during late childhood, include fatigue, muscle weakness, cramps, and recurrent carpopedal spasms (Frassetto LA. Bartter Syndrome. In: eMedicine, visited on December 3, 2017 [Link]).
Histopathology: Although renal biopsy is not usually required, histologic findings may be useful in confirming the diagnosis of Bartter syndrome. In neonatal and classic Bartter syndrome, the cardinal finding is hyperplasia of the juxtaglomerular apparatus. Less frequently, hyperplasia of the medullary interstitial cells is present. Glomerular hyalinization, apical vacuolization of the proximal tubular cells, tubular atrophy, and interstitial fibrosis may be present as a consequence of chronic hypokalemia (Frassetto LA. Bartter Syndrome. In: eMedicine, visited on December 3, 2017 [Link]).
Fibronectin glomerulopathy, which is a rare, familial glomerular disease caused by the deposition of fibronectin and other matrix-type proteins in glomeruli. Ultrastructurally, the deposits are electron-dense and usually homogenous to finely granular, occasionally showing fibrillar substructure. Fibronectin is a large dimeric glycoprotein. It functions as an adhesive glycoprotein, aiding in branching morphogenesis, cellular proliferation, wound healing, phagocytosis, platelet-platelet cohesion, and thrombus formation. Fibronectin normally exists in a soluble or plasma form (which circulates in blood) and an insoluble or cellular form (which is seen in basement membranes and extracellular matrices). Although fibronectin is found in the normal glomerular mesangial matrix, enhanced fibronectin accumulation is variably observed in several different glomerulopathies, including diabetic nephropathy and lupus nephritis. The increase in fibronectin expression in these diseases is secondary to locally stimulated mesangial and epithelial cell production of the insoluble or cellular form. By comparison, fibronectin glomerulopathy is associated with accumulation of fibronectin that is mainly derived from the soluble plasma isoform. Fibronectin glomerulopathy is rare (Rovin VH. Fibronection Glomerulopathy. In: UpToDate. Visited on December 4, 2017. [Link]).
The disorder has a slight male predominance and was originally described only in Caucasians of European descent. Subsequently, an Asian family with this disease was reported. Cases in blacks or Hispanic patients have yet to be reported. Fibronectin glomerulopathy is characterized clinically by varying degrees of proteinuria, which is typically first seen between the ages of 20 and 40 years. This is followed, over the next 15 to 20 years, by hypertension, microscopic hematuria, and, in most patients, slow progression to end-stage renal disease. Complement levels are normal. Fibronectin glomerulopathy is rarely rapidly progressive (Rovin VH. Fibronection Glomerulopathy. In: UpToDate. Visited on December 4, 2017. [Link]).
Histopathology: There is glomerular enlargement and usually some evidence of minimal cellular proliferation, producing a lobular or clover-like appearance that may be confused with membranoproliferative glomerulonephritis. Capillary walls may be thickened and the mesangium greatly expanded by acellular periodic acid-Schiff-positive (PAS-positive) homogeneous material that can result in severely narrowed capillary lumens. Staining with Congo red or methenamine silver is consistently negative. There is no specific tubulointerstitial abnormalities, however, interstitial fibrosis and tubular atrophy become more prominent over time, a common finding in progressive renal disease. (Rovin VH. Fibronection Glomerulopathy. In: UpToDate. Visited on December 4, 2017. [Link]). [Ver imagen con PAS (link)]
Electron Microscopy
There are large to massive nondescript electron-dense subendothelial and mesangial deposits. The deposits have been described as finely granular or fibrillar in some cases. If fibrillar, the fibrils are approximately 12 nm in width and 125 nm in length and are typically arranged in an irregular fashion. These fibrils are slightly wider than those seen in amyloid (8 to 10 nm). However, they are thinner than the fibrils in fibrillary glomerulonephritis (18 to 22 nm) and the microtubules of immunotactoid glomerulopathy (greater than 30 nm). (Rovin VH. Fibronection Glomerulopathy. In: UpToDate. Visited on December 4, 2017. [Link]).
Main bibliographic sources:
Additional bibliography
Homepage - - - Tutorial Index